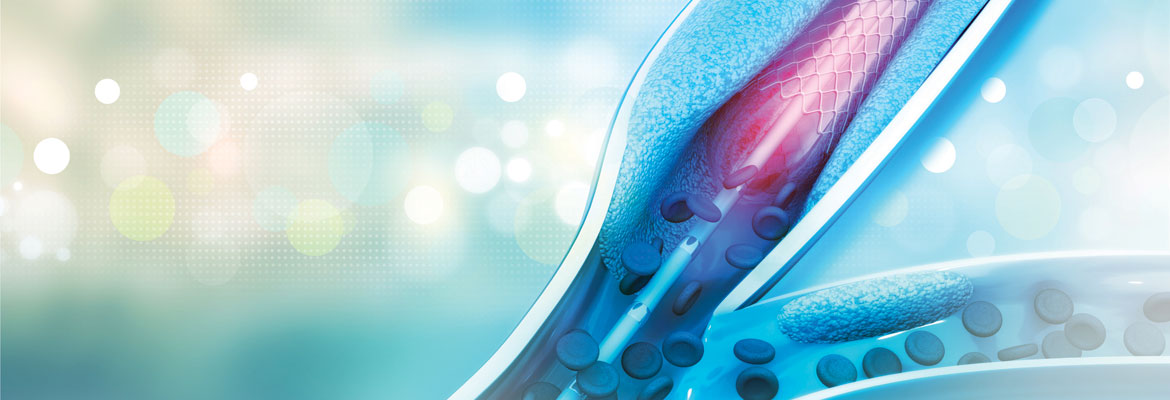
Vascular and interventional radiology at Synergy Radiology Associates offers a host of new, less invasive diagnostic and treatment options designed to minimize physical trauma to the patient, thereby reducing pain, recovery time, infection rates and the overall costs associated with surgery and hospital length of stay.
Synergy Radiology Associates offers vascular and interventional radiology services at many of the 20+ locations we operate out of throughout the Houston area including Katy, The Woodlands, Cypress, Humble and Friendswood, Webster and Kerrville, TX. Call the individual location to schedule or ask your primary care physician for a referral.
Patients who have infected fluid collections in their body may be a candidate for radiology image-guided placement of a small catheter to drain the fluid out. This can help avoid a major surgical procedure.
In this technique, the interventional radiologist inserts a very small balloon attached to a thin catheter into a blood vessel through a small nick in the skin. The catheter is threaded under X-ray guidance to the site of the blocked artery. The balloon is inflated to open the artery. Sometimes, a small metal scaffold, called a stent, is inserted to keep the blood vessel open.
Read more about Arteriogram, Angioplasty and Stenting.
When there is a blockage of the bile ducts from inflammation, gallstones or cancer, a trained interventional radiologist can bypass the obstruction with small catheters and wires under X-ray guidance. A plastic catheter is placed into the biliary tree to provide a temporary passageway for bile to drain from the liver to an external drainage bag. Sometimes a stent or catheter can be advanced into the bowel to allow internal drainage.
Read more about Biliary Drainage.
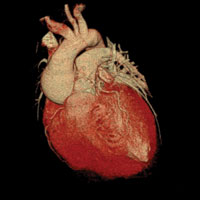
Coronary CTA is a specialized CT scan that is performed to assess a patient’s coronary arteries for atherosclerotic plaque, or hardening and plaque buildup in the arteries surrounding the heart. For some patients this test can be performed as an alternative to a heart catheterization procedure and can lend equal or better results.
Read more about Coronary CTA.
A CVAC is a tube that is inserted beneath your skin so there is a simple, pain-free way for doctors or nurses to draw your blood or give you medication or nutrients. When you have a CVAC, you are spared the irritation and discomfort of repeated needlesticks. More than 3.4 million CVACs are placed each year, and doctors increasingly recommend their use. There are several types of CVACs, including tunneled catheters (Hickman or Broviac), peripherally inserted central catheters (also called PICC lines or long lines), dialysis catheters and implantable ports.
Doctors often recommend CVACs for patients who regularly have:
- Chemotherapy treatments
- Infusions of antibiotics or other medications
- Nutritional supplements
- Hemodialysis
Read more about Central Venous Access.
This procedure is performed when the gallbladder is inflamed and surgery cannot be safely performed. A small catheter is inserted through the skin surface into the gallbladder under image guidance to allow infected bile to drain into an external collection bag.
Read more about Cholecystostomy.
Deep Vein Thrombosis (DVT) is the formation of a blood clot, known as a thrombus, in the deep leg vein. It is a very serious condition that can cause permanent damage to the leg, known as Post-Thrombotic Syndrome, or a life-threatening pulmonary embolism. The deep veins that lie near the center of the leg are surrounded by powerful muscles that contract and force deoxygenated blood back to the lungs and heart. One-way valves prevent the back-flow of blood between the contractions. (Blood is squeezed up the leg against gravity and the valves prevent it from flowing back to our feet.) When the circulation of the blood slows down due to illness, injury or inactivity, blood can accumulate or “pool,” which provides an ideal setting for clot formation.Some patients with blood clots may be candidates for interventional radiology directed placement of a catheter and use of “clot busters”.
Read more about Deep Vein Thrombosis.
A Discogram is a minimally invasive test to help doctors determine the cause of back pain. Under X-ray guidance a small needle is placed in the intervertebral disc. Contrast is injected to evaluate the disc and to help quantitate and localize the back pain. Some patients may also be candidates for a procedure called Disc Nucleoplasty where a portion of the inner part of the disk is removed by a small needle following which a thermal ablation is performed to help alleviate symptoms from bulging disks.
Read more about Discograms & Disc Nucleoplasties.
Embolization techniques employ delivery of clotting agents (coils, plastic particles, gel, foam, etc.) directly to an area that is bleeding or to block blood flow to a problem area, such as an aneurysm or a fibroid tumor in the uterus. Embolizations performed by a trained interventional radiologist can prevent major open surgeries. Small catheters and wires are guided under X-ray to perform these minimally invasive procedures. In this technique, the interventional radiologist inserts a very small balloon attached to a thin catheter into a blood vessel through a small nick in the skin. The catheter is threaded under X-ray guidance to the site of the blocked artery. The balloon is inflated to open the artery. Sometimes, a small metal scaffold, called a stent, is inserted to keep the blood vessel open.
Read more about Embolization.
Devices or fragments can sometimes dislodge within the vascular system and may need to be removed. This is performed by a trained interventional radiologist employing minimally invasive techniques with small catheters, wires and loop snare devices within the vascular system under X-ray guidance.
Read more about Foreign Body Retrieval.
Doctors often recommend placing a gastrostomy tube in the stomach for a variety of conditions in which a patient is unable to take sufficient food by mouth. In the procedure, the feeding tube is inserted through a small nick in the skin and into the stomach under X-ray guidance.
Read more about Gastrostomy & Gastrojejunostomy.
Patients who have a clot in the veins of the lower extremities and cannot be anticoagulated may need a filter placed within the inferior vena cava to prevent a pulmonary embolus. It is a tiny cage-like device that is inserted in a blood vessel to catch clots and prevent them from reaching the heart or lungs. The filter can prevent a life-threatening pulmonary embolus and can be safely placed by one of our board-certified radiologists using a neck or leg vein.
Read more about Inferior Vena Cava Filter.
Patients with osteoporosis, due to age, chemotherapy or other factors, are at increased risk for painful vertebral compression fractures. As an alternative to major surgery, these fractures can be treated by a radiologist using X-ray to guide needles in the spine fractured area, create a cavity with small balloons, and place a fast setting polymer to “internally cast” the fracture.
Download the SRA Kyphoplasty Brochure.
Read more about Kyphoplasty.
Myelograms are minimally invasive diagnostic procedures in which contrast is injected into the spinal canal under X-ray guidance. X-rays and CT images are then obtained which are interpreted by a radiologist to evaluate the spinal column, spinal cord, any major areas of disk bulging and nerve roots. Patients undergoing workup for back pain may benefit from the additional information from this procedure.
Read more about Myelograms.
Needle biopsy is a procedure performed by radiologists to identify the cause of a lump or mass, or other abnormal condition in the body. It has replaced the need for many open surgical biopsy procedures. During the procedure, the doctor inserts a small needle, guided by X-ray, CT or Ultrasound into the abnormal area. A sample of tissue is removed and given to a pathologist who looks at it under a microscope to determine what the abnormality is — for example, cancer, a noncancerous tumor, infection or scar.
Read more about Needle Biopsy.
This procedure is performed when the kidneys and ureters are blocked from stones or other other processes such as cancer or scarring. The patient is placed on their stomach and a small catheter is inserted into the skin and into the kidney under image guidance to help alleviate the obstruction.
Read more about Nephrostomy.
Pelvic congestion is a painful condition caused by enlarged or varicose veins in the pelvis. Ovarian vein embolization is performed by an interventional radiologist using image guidance and a catheter to seal off the faulty veins to prevent them from becoming enlarged and causing pain. Like UFE, ovarian vein embolization is a safe and effective outpatient procedure that is an effective alternative to open surgery.
Read more about Ovarian Vein Embolization.
Fluid within the abdominal and pelvis peritoneal cavity is removed using ultrasound guidance and a small catheter that is temporarily inserted. This procedure is performed for diagnostic or therapeutic purposes.
Read more about Paracentesis.
Peripheral Arterial Disease (PAD) – clogged or narrowed arteries in the legs – is a red flag that the same process may be going on elsewhere in the body because PAD is associated with other life-threatening vascular diseases. Through early detection, interventional radiologists can save women from future stroke, heart attack and early death. To combat this major public health issue, the Society of Interventional Radiology recommends greater screening efforts by the medical community through the use of the Ankle Brachial Index (ABI) test as well as noninvasive tests such as ultrasound. Further minimally invasive procedures such as balloon angioplasty and stenting can be performed by an interventional radiologist to help open the arteries, should the test show any blockages.
Read more about Peripheral Vascular/Arterial Disease Treatment.
Patients who need long term IV access for medicines such as chemotherapy can benefit from the placement of an implantable port. It is implanted in the skin, usually in the upper chest. A radiologist uses ultrasound or X-ray to safely guide the placement of the device under the skin and into the vascular system.
Unlike a PICC line, a port can stay in as long as you need treatment, up to several years. They do not require daily cleaning and flushing, however, they should be routinely checked and may be “declotted” when a buildup occurs in or around the port itself. When there is no longer the need for a port, it can be removed by the interventional radiologist.
Downloads/More Info:
Port Placement – Brochure
Read more about Port Placement.
The prostate is a gland that is normally the size of a walnut. With BPH, it can grow as large as a tennis ball. The enlarging prostate can put pressure on the urethra, which carries urine out of the body. This can restrict the flow of urine or, in extreme cases, cut it off completely. PAE is an outpatient procedure that requires no anesthesia. It has a high success rate (75-95%), a faster recovery, fewer complications and a lower risk of sexual side effects, such as erectile dysfunction and retrograde ejaculation.
Read more about Prostate Artery Embolization (PAE).
A pseudoaneurysm is a potentially lethal condition that can result when a catheter is placed within the femoral artery, such as during an arteriogram. Thrombin is an enzyme that causes blood to clot. An injection of thrombin into the femoral artery—guided by ultrasound—is a safe, fast and effective therapy to prevent a potentially deadly pseudoaneurysm from occurring.
Read more about Pseudoaneurysm Thrombin Injection.
Other minimally invasive therapies use the body’s own vascular tree to treat cancer. Targeted treatments can be applied via a small catheter directly to the cancer. These techniques attack the tumor from inside the body without affecting other, healthy parts of the body. Embolization effectively cuts off the blood supply feeding the tumor. An interventional radiologist places a small catheter into the arteries feeding the tumor and injects tiny embolization particles that lodge in smaller vessels and prevent blood from reaching the tumor.
Radioembolization is a relatively new procedure that uses tiny particles containing a high dose of localized radiation to destroy tumors while minimizing the effect on healthy tissue.
Read more about Radioembolization.
A minimally invasive treatment for cancer, RFA uses imaging techniques such as ultrasound, CT or MRI to guide a needle electrode into a cancerous tumor. High-frequency electric currents passed through the electrode create heat that destroys the cancerous cells.
Read more about Radiofrequency Ablation for Liver and Kidney Cancer.
Facet joint and nerve root blocks are minimally invasive X-ray guided procedures performed by a radiologist to alleviate pain in patients by selectively injecting anti-inflammatory agents around the spinal facet joints or around the adjacent spinal nerves.
Read more about Spine Facet Joint & Nerve Root Blocks.
Steroid injections are minimally invasive X-ray-guided procedures performed by Synergy Radiology Associates’ board-certified radiologists to alleviate pain, most often in the spine and joints. Anti-inflammatory agents are injected directly into the targeted area. This can be performed in patients who suffer pain caused by bulging disks, stenosis of the spine or post-operative surgery syndromes. Additionally, steroid injections can be used to alleviate degenerative joint pain such as in the hips or knees.
Downloads/More Info:
Spinal Steroid Injections – Brochure
Read more about Steroid Injections.
Male patients with symptomatic enlarged testicular or scrotal veins, called varicoceles, may benefit from minimally invasive catheter directed embolization. Pooling of blood in the veins of the scrotum, causes them to enlarge. The internal pressure and temperature may increase, possibly damaging the testicles and decreasing fertility. Symptoms of varicocele can include abnormal enlargement of veins in scrotum, dull ache or pain in the scrotum.
This condition can be treated through a minimally invasive procedure called Testicular Vein Embolization or Varicocele Embolization. During the procedure, a catheter is inserted into a blood vessel in the groin, and advanced to the site of the varicocele. A special coil is then inserted to embolize (block) the vein, stopping abnormal blood flow, reducing the pressure in the veins and diverting it to other, healthy veins. Eventually, the enlarged vein will shrink and disappear. Patients are generally able to leave the hospital within a few hours of the procedure, with minimal recovery time.
Read more about Testicular Vein Embolization.
Patients who have fluid building up around their lung can benefit from drainage of the fluid for symptom relief and for diagnostic purposes. A radiologist can use Ultrasound to guide a needle where the fluid is to safely drain.
Read more about Thoracentesis.
This treatment for cancer uses imaging guidance to identify blood vessels that supply blood to a tumor, followed by the injection of anti-cancer drugs (chemotherapy) directly into the blood vessel. This technique “traps” the chemotherapy in the tumor while minimizing the effect of the drugs on other, healthy areas of the body.
Read more about Transarterial Chemoembolization (TACE).
Recent advances in targeted tumor therapy give patients and their physicians excellent options for treating primary or metastatic cancer. Thermal ablation uses extreme heat to treat cancer. Using imaging guidance, thin probes are advanced through the skin directly into a tumor to destroy or “ablate” the tumor. Radiofrequency, cryoablation or microwave are minimally invasive options for patients with primary and metastatic cancers, including cancers of the kidney, lung, bone and liver.
Radiofrequency ablation (RFA) is used to treat tumors in the lungs, liver, kidneys, bones and other organs. During treatment, a special probe is placed inside the tumor. Radiofrequency waves passing through the probe increase temperature within the tumor and destroy it. RFA can be used with small primary tumors and metastasized tumors.
Cryoablation (aka cryosurgery, cryotherapy) kills cancer cells using extreme cold. A cryoprobe is inserted into the tumor where a freezing and thawing process is repeated several times. It is used to treat cancer throughout the body, and uses liquid nitrogen, liquid nitrous oxide or compressed argon gas as a cooling agent. After the procedure, the frozen tissue thaws and is absorbed by the body.
Microwave ablation (MWA) uses electromagnetic waves to heat and destroy cancer cells. It is generally used for patients who are not eligible for surgery for primary or secondary lung, liver, renal, adrenal and bone malignancies. Unlike RFA, MWA does not rely on an electrical circuit; therefore multiple applicators can be used simultaneously.
Read more about Tumor Ablation.
Patients who have recurring pleural fluid (excess fluid in the abdomen) can have issues breathing, chest pain, coughing and discomfort. A tunneled pleural catheter is a tube placed under the skin within the chest to help relieve these symptoms. The pleural fluid is drained by the patient at home using a collection system, avoiding numerous trips to the doctor.
Read more about Tunneled Pleural Catheter.
Patients with blockage of the ureters may benefit from internal plastic stents which can be placed by an interventional radiologist under X-ray guidance.
Read more about Ureteral Stent Placement.
For men with suspicious prostate cancer findings, including positive digital rectal exams (DRE) and elevated PSA (prostate-specific antigen) levels, the UroNav Fusion Biopsy System (also called MRI/TRUS fusion biopsy) combines MRI images with real-time ultrasound to help better assist the Urologist who will be performing the biopsy. Through UroNav technology, the Urologist has a much more accurate and clearly defined area for performing the biopsy – leading to more accurate and beneficial results.
Read more about UroNav Fusion Biopsy.
Read how SRA uses hi-tech, 3-D imaging for better prostate cancer diagnosis here.
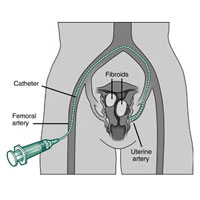
Many women develop uterine fibroid tumors as they age or after childbirth. The tumors can also be hereditary. Fibroid tumors are benign tumors that cause extreme bleeding, pain and extreme discomfort in women. Through Uterine Fibroid Embolization (also known as Uterine Artery Embolization), an interventional radiologist is able to guide small catheters to the arteries that supply the blood flow to the tumors and cut off the blood supply. This causes the tumors to shrink and symptoms to significantly fade, almost immediately. UFE is often performed as an alternative to myomectomy or hysterectomy, as it is minimally invasive with the risks being much smaller and the recovery time being much shorter.
Downloads/More Info:
UFE – A Less Invasive Way to Treat Uterine Fibroids – Brochure
Uterine Fibroids: What Are My Options? – Flyer
Read more about Uterine Fibroid Artery Embolization (UFE).
Under real-time X-ray guidance, called fluoroscopy, contrast is injected in a vein in order to detect an abnormality, such as a narrowing or blockage. The abnormality can sometimes be treated with balloon angioplasty or stenting.
Read more about Venogram.
A form of radiation therapy to treat cancer that cannot be treated surgically, such as hepatic cell carcinoma, liver cancer or metastatic cancer. The treatment involves the injection of tiny microspheres of radioactive material into the arteries that supply the tumor.
Read more about Y90 Selective Internal Radiation Therapy.
